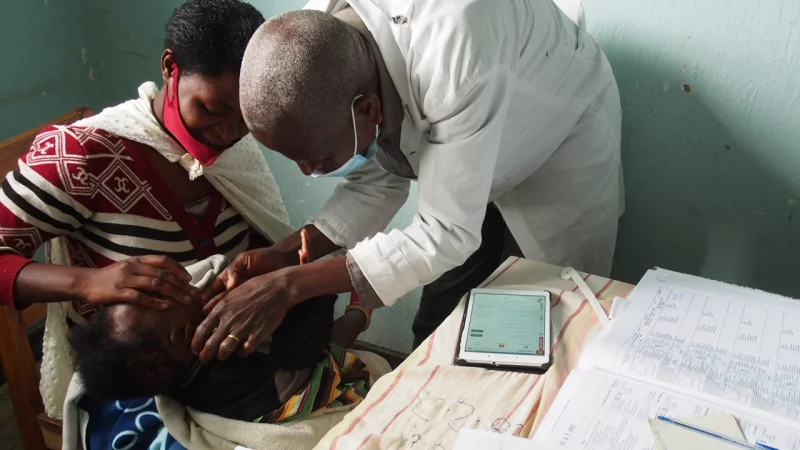
Healthcare providers in rural Rwanda face enormous daily pressure. In many clinics, nurses treat dozens of patients every day, often working with limited diagnostic tools and minimal time to evaluate complex symptoms. Under these circumstances, prescribing antibiotics can sometimes become the default response when the cause of illness is uncertain.
This widespread pattern has contributed to growing concern about antibiotic overuse. Medical researchers and public health authorities warn that excessive prescriptions can accelerate antimicrobial resistance, a global health threat in which bacteria evolve to withstand existing treatments.
A new digital system designed for frontline healthcare workers is beginning to change that dynamic. The tablet-based clinical support tool, known as ePOCT+, provides step-by-step guidance to help clinicians assess symptoms, determine likely diagnoses, and recommend treatments more accurately.
Rural Clinics Face Pressure and Diagnostic Challenges
In many rural health facilities across Rwanda, healthcare workers manage large numbers of patients in a single day. Adults and children often travel long distances to reach clinics, seeking help for fevers, respiratory infections, injuries, or other illnesses.
With limited laboratory resources and time constraints, clinicians frequently rely on precautionary prescribing. Antibiotics are often given even when the illness may be caused by viruses, which do not respond to such medication. Over time, this practice contributes to the global crisis of antimicrobial resistance highlighted by organizations such as the <a href="/es/”https://www.who.int”/">World Health Organization</a>.
Researchers studying prescription patterns across 32 clinics in Rwanda found that approximately 71% of pediatric visits resulted in an antibiotic prescription before the introduction of the digital tool. Many of these prescriptions were likely unnecessary, particularly in cases involving viral infections.
While a single unnecessary prescription might not seem harmful, the cumulative impact across communities can be significant. Overuse increases the risk that bacteria will develop resistance to commonly used drugs, making infections more difficult and expensive to treat in the future.
The issue is especially pressing in regions with limited healthcare infrastructure, where losing the effectiveness of antibiotics could severely affect patient outcomes.
A Tablet-Based System Offers Clinical Guidance
To address these challenges, researchers developed ePOCT+, a clinical decision-support system that runs on a tablet computer. The tool translates complex medical guidelines into an interactive step-by-step process designed for use during patient consultations.
Instead of consulting multiple paper manuals, clinicians can input symptoms and vital signs directly into the device. The system analyzes the information using a medical algorithm based on internationally recognized treatment guidelines and diagnostic standards developed by institutions including the <a href="/es/”https://www.cdc.gov”/">Centers for Disease Control and Prevention</a>.
During a consultation, a nurse may enter information about fever, breathing rate, oxygen levels, or other symptoms. The system then guides the clinician through additional checks before suggesting a likely diagnosis. For respiratory illnesses, for example, the algorithm helps differentiate between viral pneumonia and bacterial pneumonia.
Only bacterial cases are recommended for antibiotic treatment. This structured process typically takes about 10 minutes and provides healthcare workers with a digital second opinion while they examine the patient.
Training healthcare workers to use the system proved relatively simple. In many clinics, staff members were able to learn the process within a single day of hands-on practice.
Significant Drop in Antibiotic Prescriptions
After introducing ePOCT+ across the participating clinics, researchers monitored nearly 60,000 patient visits to evaluate the system’s impact. The results showed a substantial reduction in antibiotic prescribing.
Prescription rates dropped from 71% of pediatric visits to roughly 25%, a dramatic improvement that still maintained safe health outcomes for children. The findings demonstrated that reducing unnecessary antibiotics did not lead to an increase in complications or untreated infections.
In addition to improving prescribing practices, the digital system also helped clinicians detect conditions that might otherwise go unnoticed, including malnutrition and anemia. Early identification of these problems allows for more targeted treatment and better long-term patient care.
Health authorities in Rwanda are exploring ways to integrate similar tools into broader national health systems. The country has been expanding its digital health infrastructure with initiatives supported by institutions such as the <a href="/es/”https://www.moh.gov.rw”/">Rwanda Ministry of Health</a>.
At the same time, health economists note that reducing unnecessary prescriptions could generate financial savings for the country’s public insurance system. Managing antibiotic resistance is also a priority for global health initiatives supported by organizations like the <a href="/es/”https://www.gavi.org”/">Gavi, the Vaccine Alliance</a>, which works to improve access to healthcare solutions in lower-income regions.
As digital health technologies continue to evolve, tools that support frontline clinicians may play a growing role in protecting the effectiveness of antibiotics and improving diagnostic accuracy in healthcare systems with limited resources.